|
The nurse’s role is to strike a balance between the two through open discussion, sharing information with the patient, and negotiation. BeneficenceĪutonomy (respecting a patient’s wishes) and beneficence (doing good), two fundamental ethical principles in nursing, are sometimes in conflict. In some cases, a patient’s right to autonomy may directly conflict with what nurses or other health care workers believe is best. This includes a patient’s right to refuse medications, treatments, or procedures. Patient autonomy - the right of patients to independently make decisions about their care based on their personal or cultural beliefs and values - is a paramount principle of nursing. 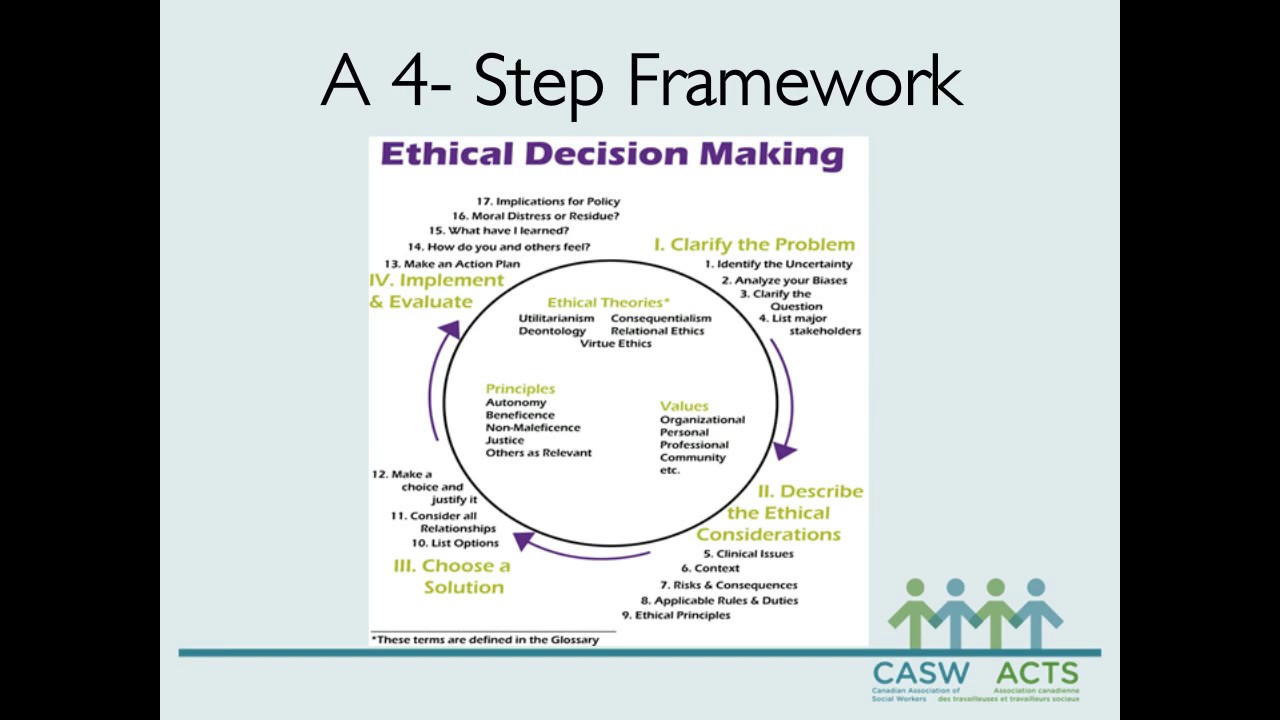
The second and third provisions specifically address the nurse’s role in protecting patients’ rights and best interests. 
The first three provisions of the Code of Ethics for Nurses deal directly with the nurse’s relationship with their patient. Below are some common dilemmas that nurses may face and how to navigate them. The Code and its accompanying provisions lay out the values and commitments nurses are expected to uphold, identify the boundaries of duty and loyalty, and describe the broader responsibilities nurses have outside of patient care.Īn advanced degree, such as an online Master of Science in Nursing, can help aspiring nurses identify and address many ethical dilemmas in nursing. The Code is a living document, regularly updated to reflect modern-day advancements and challenges, and represents the social contract between nurses and the public. These kinds of ethical dilemmas often challenge nurses to deliver optimal patient care while also adhering to professional boundaries.Įthical values are so fundamental to nursing that the American Nurses Association (ANA) established a formal Code of Ethics for Nurses - often referred to simply as “The Code” - in the 1950s to set goals and values for the profession as a whole and to serve as a guide for nurses in their daily practice. These dilemmas can take different forms, such as how best to respect a patient’s decision to refuse treatment due to cultural or personal beliefs, or what to do when conflicts arise between patients and their families in making end-of-life care decisions. Therefore, the author would provide patient-centered care and act according to the patient’s request for comfort measures.Nurses frequently face ethical dilemmas while caring for their patients. Moreover, patients/caregivers are aware that care provision in this facility is comfort, as the client’s condition can no longer be cured (Tavares et al., 2016). The author’s stance on this issue is to continue providing comfort and evaluate the benefits of such measures to the patient. Some nurses question whether it is morally acceptable to be administering medications, such as morphine, that could produce respiratory distress in someone that already has breathing difficulties (Vries & Plakosta, 2017). 
The ethic al dilem ma that nurses encount er is quest ionin g wheth er these pharmacol ogic treat ments enhance the deteriorating conditions the clients are in, therefore hastening death. On e of th e ma in go al s in pa ll ia ti ve ca re is to fa ci li ta te a “p ea ce fu l de at h” by admin iste ring sedat ing and “comfo rtin g” medica tions (Vries & Plasko ta, 2017).
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
